Summit Eye Center Blog
Glaucoma - What is it? Am I at risk? How is it treated?
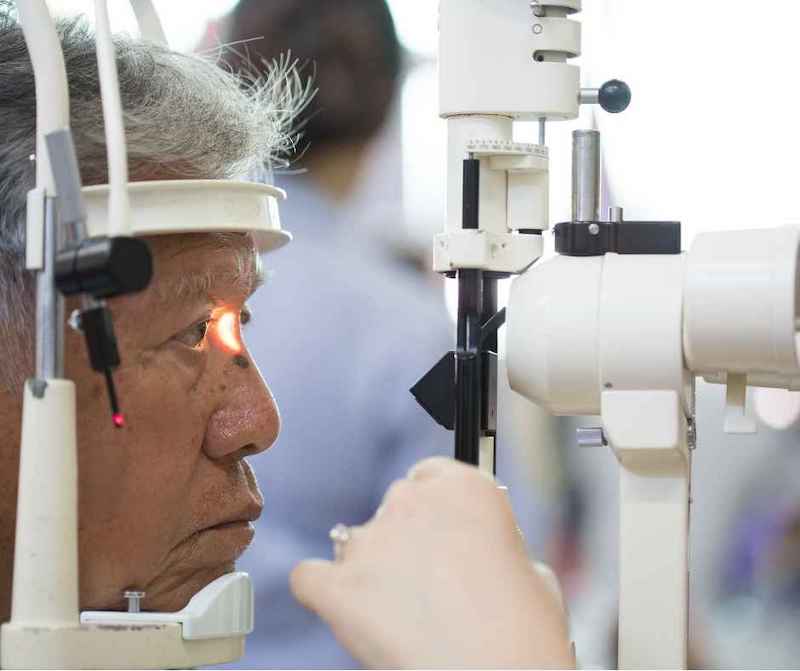
Glaucoma Awareness Month is drawing to a close. This blog will provide some information on what glaucoma is, how it is tested for, who is at increased risk and how it is treated.
What is glaucoma?
Glaucoma is a disease that affects the optic nerve in the back of our eye. This nerve is responsible for transmitting the visual information from our eye to the occipital lobe, the back of our brain, where it is processed into the images that we see. Damage to this nerve tissue results in blind spots in one’s vision. If left untreated, glaucoma can result in total blindness.
Initially, glaucoma does not have any symptoms. Because of this it is often called “the silent thief of sight”. Therefore, regular dilated eye exams are critical to its diagnosis. During this exam, your doctor carefully exams the optic nerve’s appearance with special lenses and a microscope. If any irregularity is noticed, the doctor will likely then order some special tests to look closer for any possible signs of glaucoma. These tests include, but are not limited to those listed below.
Glaucoma tests
Optical coherence tomography (OCT) uses light waves to take a cross-section of the retina and the optic nerve head in the back of the eye. This allows the measurement of the thickness of the nerve tissue in the back of the eye. These measurements are then compared to people your age without glaucoma.
Visual field testing involves a dome-shaped machine that you will look into. There will be a fixation light in the center of the bowl that you will focus on. Then, randomly dim lights will be flashed in your peripheral or side vision. You will click a button when you see these lights. The machine will keep track of the location and intensity of the lights that you missed. Your results are compared to people your age without glaucoma.
Pachymetry is a test that measures the thickness of the cornea, the clear layer over the colored part of the eye. People with thinner corneas have a higher risk of developing glaucoma.
Intraocular pressure is the pressure within the eye. People with a higher pressure are at an increased risk of glaucoma. It was once thought that you needed an elevated pressure to have glaucoma, but research shows that as many as 30-40% of people with glaucoma never have an elevated eye pressure.
Electroretinography (ERG) provides a measurement of the functioning of the retinal ganglion cells in the back of the eye. These are the cells that are responsible for taking the visual information from the light that enters the eye and transmitting it to the brain via the optic nerve. Glaucoma results in the death of these cells over time. Once dead, these cells are unable to regenerate or be replaced.
Gonioscopy involves the use of a special lens to look at the drainage area of the eye, the angle. Certain conditions such as trauma or pigment dispersion syndrome can cause irregularities within the drainage system that can lead to the development of glaucoma.
Optic nerve photos are, just it sounds, pictures of the optic nerve head that are used for comparison to monitor for change over time.
Who is at risk for glaucoma?
• Age over 40
• Family history of glaucoma
• African American, Hispanic or Asian heritage
• Elevated eye pressure
• Thin corneal thickness
• History of an eye injury
• History of long-term steroid use
How is glaucoma treated?
Glaucoma is treated by lowering one’s eye pressure. It has been shown that whether you start with an elevated pressure or a pressure that is within the normal range, lowering one’s pressure from where it is naturally is effective at treating glaucoma.
The first line treatment for glaucoma is typically either an eye drop that you use once a day at night to lower the pressure or an office-based laser procedure called SLT, selective laser trabeculoplasty.
If additional lowering of the pressure is needed, there are numerous classes of medication eye drops that can be used to drive the pressure lower.
There are also surgical procedures that can be used at the same time as cataract surgery called minimally invasive glaucoma surgery, MIGS. These procedures offer increased lowering of one’s eye pressure with minimal side effects or risk.
If the above treatment options are not enough to get the pressure where it needs to be, trabeculectomy or tube shunt surgery can be employed to attempt to get the pressure as low as possible.
In summary, glaucoma is a treatable eye condition. It is important to catch it at an early stage before a person is symptomatic of any visual change related to glaucoma damage. It is also important to use the medication eye drops at the frequency prescribed by your doctor. Medications tend to wear off over time. Therefore, missing doses of your eye drops allows the eye pressure to creep back up. Fluctuations in one’s eye pressure has been linked to progression of glaucoma damage is several clinical studies.
Summit Eye Center specializes in the treatment of glaucoma. We provide clinical management with all of the diagnostic testing listed earlier in this blog. We also offer selective laser trabeculectomy, SLT, to those patients that it is appropriate for. MIGS procedures such as the iStent Inject from Glaukos, ab-interno canaloplasty (ABiC) with the Ellex system and the Hydrus microstent from Ivantis are also considered for appropriate patients.
If you would like to schedule a comprehensive eye exam or a glaucoma evaluation, call 816-246-2111 or email
