Summit Eye Center Blog
Keratoconus
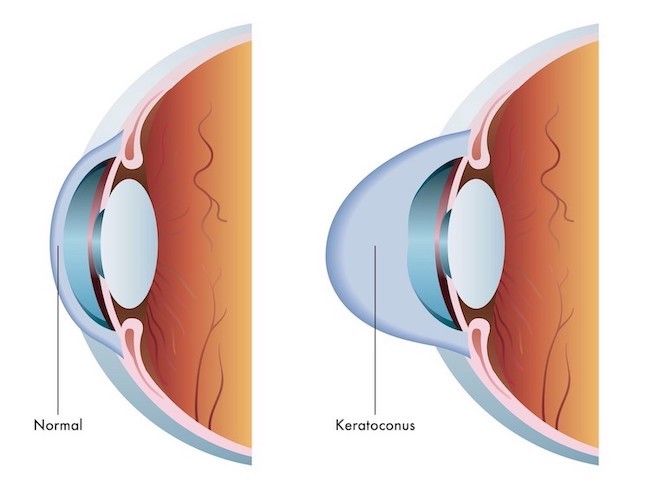
Keratoconus (KC) is a condition that affects the cornea. The cornea is the clear, dome-shaped tissue that sits above the iris, the colored part of the eye, and the pupil. The cornea focuses light as it enters the eye and then travels through the pupil to be focused on the retina in the back of the eye.
With KC, there is a progressive thinning and bulging of the cornea, which results in irregular astigmatism. This irregularity in the curvature of the cornea causes blurry or distorted vision that can affect one’s ability to read or drive.
Keratoconus typically develops during childhood and progresses into adulthood. It will progress at different rates from individual to individual. Each eye of a person can also progress at different rates.
The incidence of KC in the general population varies from 1 in 2000 to 1 in 500 depending on the study. This variance is probably related to recent studies that have used technology that can better pick up early signs of KC, resulting in an incidence of 1 in 500.
What causes keratoconus?
 It is not known for sure what causes KC but it is likely due to a combination of genetic and environmental factors. Approximately 1 in 10 patients with KC have a family history of the condition. It has also been linked to eye rubbing and allergies. This eye rubbing is often with one’s knuckles or fingertips pushing firmly onto the eyes. Sleeping with one’s face against a pillow has also been linked to KC. The mechanical stress of eye rubbing is thought to result in a rearrangement of collagen fibers as well as an increase in tear film collagenases that leads to corneal thinning and bulging.
It is not known for sure what causes KC but it is likely due to a combination of genetic and environmental factors. Approximately 1 in 10 patients with KC have a family history of the condition. It has also been linked to eye rubbing and allergies. This eye rubbing is often with one’s knuckles or fingertips pushing firmly onto the eyes. Sleeping with one’s face against a pillow has also been linked to KC. The mechanical stress of eye rubbing is thought to result in a rearrangement of collagen fibers as well as an increase in tear film collagenases that leads to corneal thinning and bulging.
What are symptoms of keratoconus?
Early symptoms of KC include blurry or distorted vision. There may be some increased light sensitivity. As KC progresses, the level of blurriness and distortion will increase. Patients will often notice “ghosting” of images. Those with advanced KC may also experience discomfort wearing contact lenses.
How is keratoconus diagnosed?
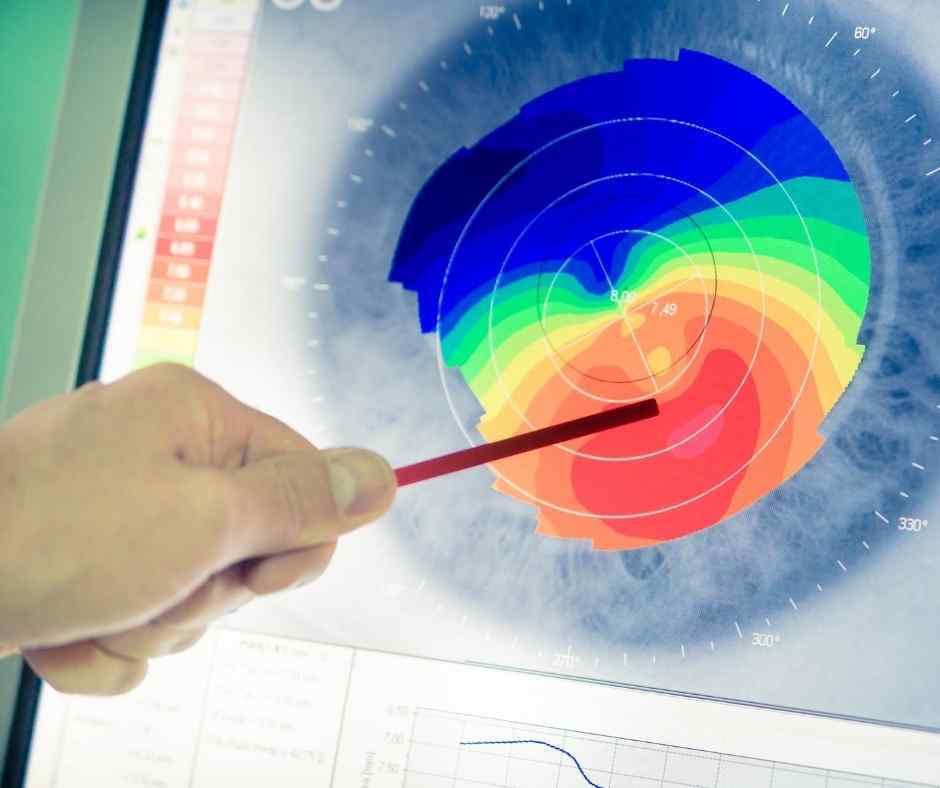 The most common test done to diagnose KC is corneal topography. This test provides the doctor with a topographical map of the curvature of the cornea. Measurements of the thickness of the cornea will also aid in the diagnosis of KC, as these patients have a thinning of the cornea. Taking that one step further, doctors can also look at the thickness of the outer layer of the cornea, the epithelium. Epithelial thinning may be the most sensitive way to pick up signs of KC in its earliest stages.
The most common test done to diagnose KC is corneal topography. This test provides the doctor with a topographical map of the curvature of the cornea. Measurements of the thickness of the cornea will also aid in the diagnosis of KC, as these patients have a thinning of the cornea. Taking that one step further, doctors can also look at the thickness of the outer layer of the cornea, the epithelium. Epithelial thinning may be the most sensitive way to pick up signs of KC in its earliest stages.
If there is one thing to take away from this, it is...DON’T RUB YOUR EYES!
If you feel the urge to rub your eyes, talk to your eye doctor for possible solutions such as allergy treatment to minimize the temptation to rub your eyes.
The doctors of Summit Eye Center focus on the diagnosis and treatment of keratoconus. Our next blog will feature discussion on the treatment of KC. If you have any questions regarding KC or other eye conditions, call us at 816-246-2111 or email
